Peripheral Artery Disease Symptoms — Why Leg Pain While Walking Is a Warning Sign
Peripheral Artery Disease Symptoms — Why Leg Pain While Walking Is a Warning Sign
 Peripheral artery disease symptoms are one of the most under-recognised warning signs in Indian medicine — and in the diabetic population, which is enormous across UP, Delhi NCR, and the surrounding regions, peripheral artery disease often presents with no warning at all until the disease is critical. Dr. Ved Prakash, Director of CTVS and Vascular Surgery at Yatharth Super Speciality Hospitals, Greater Noida, explains what peripheral artery disease is, the stages of symptoms from mild to limb-threatening, and when intervention is urgently needed.
Peripheral artery disease symptoms are one of the most under-recognised warning signs in Indian medicine — and in the diabetic population, which is enormous across UP, Delhi NCR, and the surrounding regions, peripheral artery disease often presents with no warning at all until the disease is critical. Dr. Ved Prakash, Director of CTVS and Vascular Surgery at Yatharth Super Speciality Hospitals, Greater Noida, explains what peripheral artery disease is, the stages of symptoms from mild to limb-threatening, and when intervention is urgently needed.
What Is Peripheral Artery Disease?
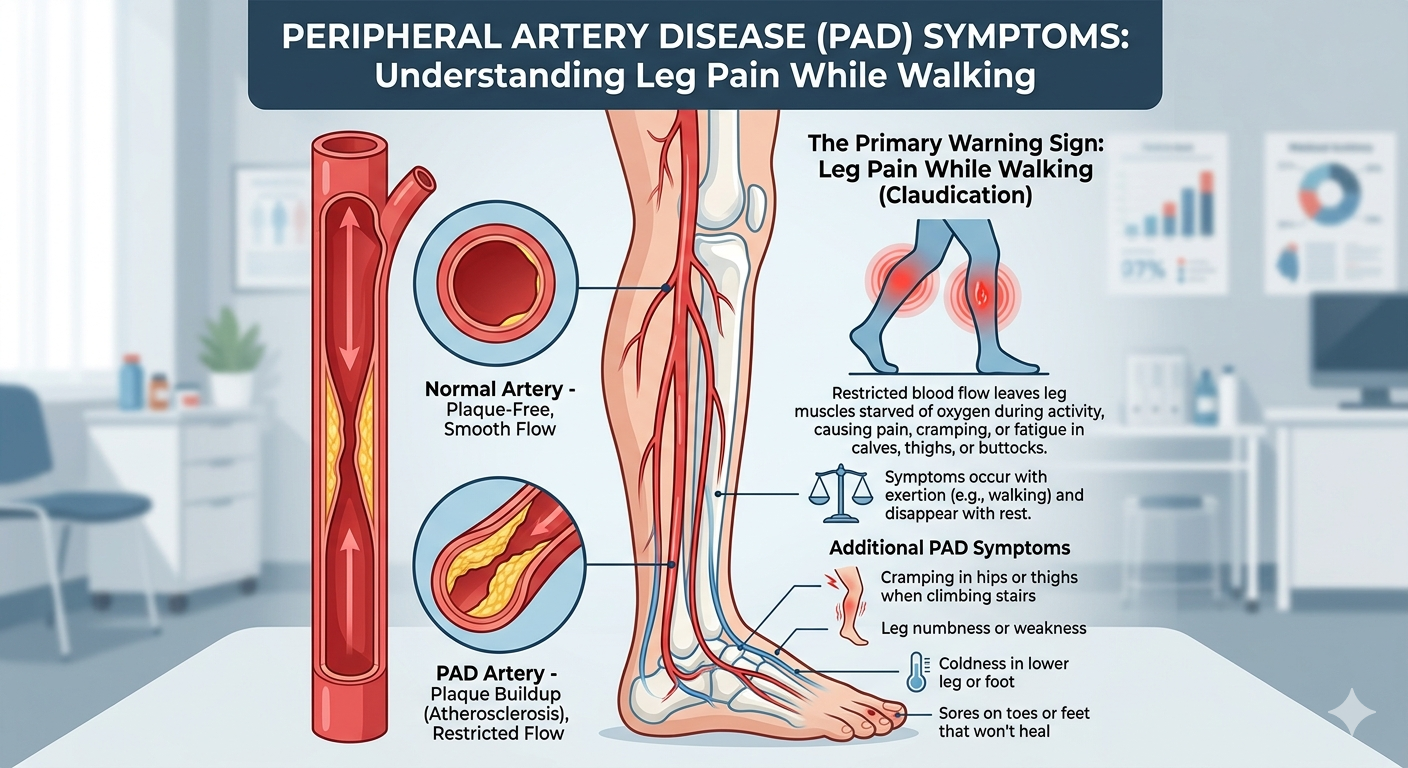
Peripheral artery disease (PAD) is atherosclerosis — plaque buildup — affecting the arteries that supply blood to the legs. It is the same disease process as coronary artery disease in the heart, occurring in a different location. As the arteries narrow, the leg muscles do not receive enough blood during exercise — and as the disease progresses, not even at rest. PAD affects approximately 200 million people worldwide and is significantly underdiagnosed in India.
PAD is not the same as deep vein thrombosis or varicose veins. Those are venous (vein) problems. PAD is an arterial (artery) problem — it is about blood not reaching the leg, not blood failing to drain from it. The distinction matters because the symptoms, investigations, and treatments are completely different. For comparison, read about deep vein thrombosis.
Peripheral Artery Disease Symptoms — Stage by Stage
Stage 1 — Claudication
The hallmark PAD symptom. Cramping, tightness, or aching in the calf, thigh, or buttock that comes on after a predictable walking distance — say, 300 metres — and stops you in your tracks. After 5–10 minutes of standing still, the pain disappears completely. You can then walk again — until the same distance is reached.
The location of the pain tells you the level of arterial disease: calf claudication means disease in the superficial femoral artery (mid-thigh level); thigh and buttock claudication means disease in the iliac arteries of the pelvis.
Claudication is often written off as arthritis, age-related muscle weakness, or sciatica — none of which share its specific pattern of predictable onset with walking and complete relief with rest.
Stage 2 — Worsening Claudication
As peripheral artery disease progresses without treatment, the claudication distance shortens. A patient who could walk 500 metres two years ago now manages 100. This reflects worsening arterial narrowing and is the signal that intervention should be considered before the next stage develops.
Stage 3 — Rest Pain
When peripheral artery disease becomes severe enough, the foot no longer receives adequate blood even lying in bed. The patient experiences burning or aching pain in the foot and toes — classically worse at night, and relieved slightly by hanging the foot over the edge of the bed (gravity assists blood flow). Rest pain is a medical emergency. Without treatment, tissue loss — gangrene — follows within weeks.
Stage 4 — Tissue Loss (Ulceration or Gangrene)
The most advanced peripheral artery disease symptom. Wounds on the foot or toes that do not heal despite weeks of dressing, or areas of blackened, dry or wet gangrene. In diabetic patients, this is often the first and only presentation of peripheral artery disease — because diabetic neuropathy has eliminated the earlier pain warning signals entirely.
Peripheral Artery Disease in Diabetic Patients — The Silent Crisis
This is the most important section for a significant proportion of readers across western UP and Delhi NCR, where diabetes rates are among the highest in the country.
Diabetic neuropathy — nerve damage from chronic high blood sugar — destroys the pain sensation in the feet and lower legs. A diabetic patient with PAD advanced enough to cause rest pain may feel nothing. A small cut on the foot from a tight shoe may go unnoticed for days. A wound that should heal in a week sits open for months — because the blood supply needed for healing is not arriving. By the time a diabetic patient presents to a vascular surgeon with a non-healing foot wound, they often have severe, critical peripheral artery disease that has been silently progressing for years.
Annual ABI (Ankle-Brachial Index) measurement is recommended for all diabetic patients over 50. It takes five minutes, is completely painless, and can detect PAD before any symptoms develop.
How Is Peripheral Artery Disease Diagnosed?
- ABI (Ankle-Brachial Index): Blood pressure cuff at the ankle compared to the arm. A ratio below 0.9 confirms PAD. Below 0.5 indicates critical ischaemia. Fast, painless, available in any vascular clinic.
- Duplex Doppler ultrasound: Maps the arterial anatomy and identifies narrowings without radiation or dye.
- CT angiography: Detailed 3D imaging from the aorta to the foot — essential before planning angioplasty or bypass surgery.
- Conventional angiography: Catheter-based — performed in the interventional suite when treatment is planned immediately.
Peripheral Artery Disease Treatment
Medical management: Antiplatelet drugs (aspirin or clopidogrel), statin therapy, strict blood pressure and blood sugar control, and smoking cessation. Supervised walking exercise programmes — counterintuitive but effective — can increase the claudication distance by 50–100% in 3 months.
Endovascular treatment (angioplasty/stenting): A catheter opens the narrowed artery and a stent holds it open. Minimally invasive, 1–2 day hospital stay, faster recovery.
Peripheral bypass surgery: For long or multiple blockages not amenable to angioplasty — a vein or synthetic graft bypasses the blocked arterial segment. More invasive but durable, with recovery of 4–6 weeks.
For patients with critical limb ischaemia or a non-healing diabetic foot wound, peripheral vascular disease treatment in Delhi NCR at Yatharth Hospital is available on an urgent basis — WhatsApp your clinical photos and report to +91-9355255106 for a rapid pre-assessment.
Frequently Asked Questions — Peripheral Artery Disease Symptoms
What is the most common symptom of peripheral artery disease?
Claudication — leg cramping that starts after a predictable walking distance and disappears completely with 5–10 minutes of rest. It affects about 50% of PAD patients; the other half are asymptomatic, particularly diabetics.
Why are diabetic patients at higher risk?
Diabetes doubles PAD risk and eliminates the pain signals (via neuropathy) that would normally alert patients. A diabetic with severe PAD may have no leg pain — their first sign is a foot wound that will not heal. Annual ABI screening is essential for all diabetics over 50.
What is claudication and how is it different from sciatica?
Claudication is vascular — predictable onset with walking, complete relief in minutes with rest, worsens going uphill. Sciatica is neurological — varies with position, not relieved by standing still, radiates from the back. Both can coexist.
When does peripheral artery disease require surgery?
When rest pain is present, when any tissue loss (ulceration or gangrene) has occurred, or when claudication prevents basic daily activity despite medical treatment. These stages are classified as critical limb ischaemia and require urgent intervention to prevent amputation.
Dr. Ved Prakash | Director, CTVS — Yatharth Super Speciality Hospitals, Greater Noida
📞 +91-9355255106 |
📧 drvedprakash@gmail.com |
Book Appointment →


