DVT (Deep Vein Thrombosis) — Warning Signs, Risk Factors and Treatment
DVT (Deep Vein Thrombosis) — Warning Signs, Risk Factors and Treatment
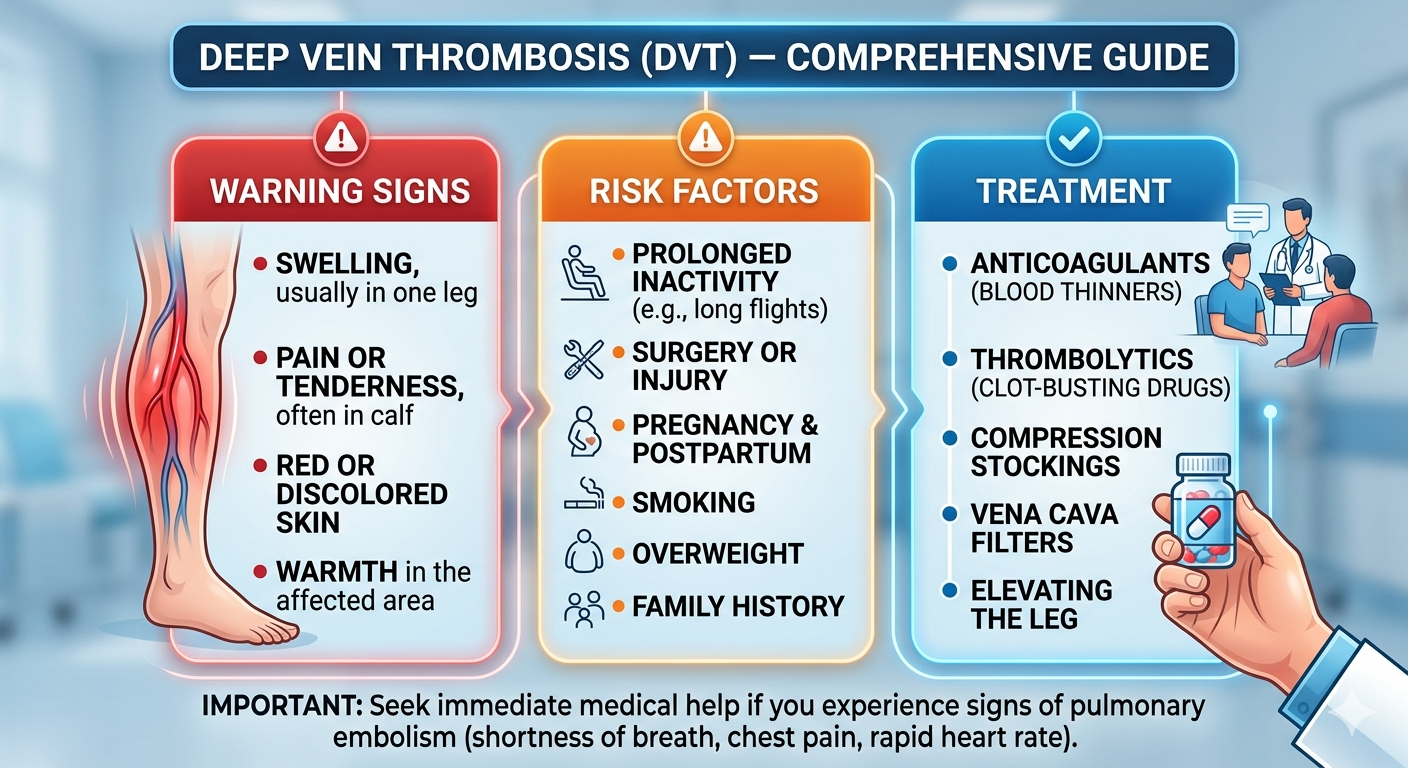
DVT — deep vein thrombosis — is a blood clot in the deep veins of the leg, and its symptoms are dangerously easy to ignore or mistake for a muscle problem. What makes DVT particularly serious is not the clot in the leg itself — it is what happens when a fragment breaks off and travels to the lungs. That is a pulmonary embolism, and it can be fatal within minutes. Dr. Ved Prakash, Director of CTVS and Vascular Surgery at Yatharth Super Speciality Hospitals, Greater Noida, explains DVT deep vein thrombosis symptoms, who is most at risk, and what treatment involves.
What Is DVT — Deep Vein Thrombosis?
Deep veins are the major vessels that carry blood from the legs back to the heart. When a clot forms in one of these deep veins — most commonly in the calf, thigh, or pelvis — blood cannot drain normally from the affected leg. The result is the swelling, pain, and warmth that characterise DVT deep vein thrombosis symptoms. And because the deep veins are connected directly to the pulmonary circulation, a piece of the clot can detach and reach the lungs at any time.
DVT Deep Vein Thrombosis Symptoms — What to Look For
Unilateral (One-Sided) Leg Swelling
DVT almost always affects one leg. Swelling of both legs together is rarely caused by DVT — it more commonly indicates heart failure or low albumin. If one calf or thigh is noticeably larger than the other and this developed over hours or a few days, DVT must be ruled out urgently.
Calf Pain and Tenderness
Aching or tenderness in the calf — often mistaken for a muscle strain or cramp. The pain is typically worse when walking and when the foot is flexed upward (Homan’s sign — though this is not reliable as a standalone test). Many patients describe it as a persistent heaviness or soreness that does not improve with rest the way a muscle injury would.
Warmth and Redness
The skin over the clotted vein may feel warm to the touch and appear reddish or purplish — caused by the inflammatory response to the clot. This can look similar to cellulitis, which is a skin infection. DVT and cellulitis require completely different treatments, so a duplex ultrasound — not antibiotics alone — is always needed when the diagnosis is uncertain.
Distended Surface Veins
When the deep vein is blocked, blood reroutes through the surface veins — which then become visibly distended. This is different from pre-existing varicose veins and appears more suddenly.
If you have sudden breathlessness, sharp chest pain, or are coughing blood — go to a hospital emergency immediately. These are pulmonary embolism symptoms and require urgent treatment.
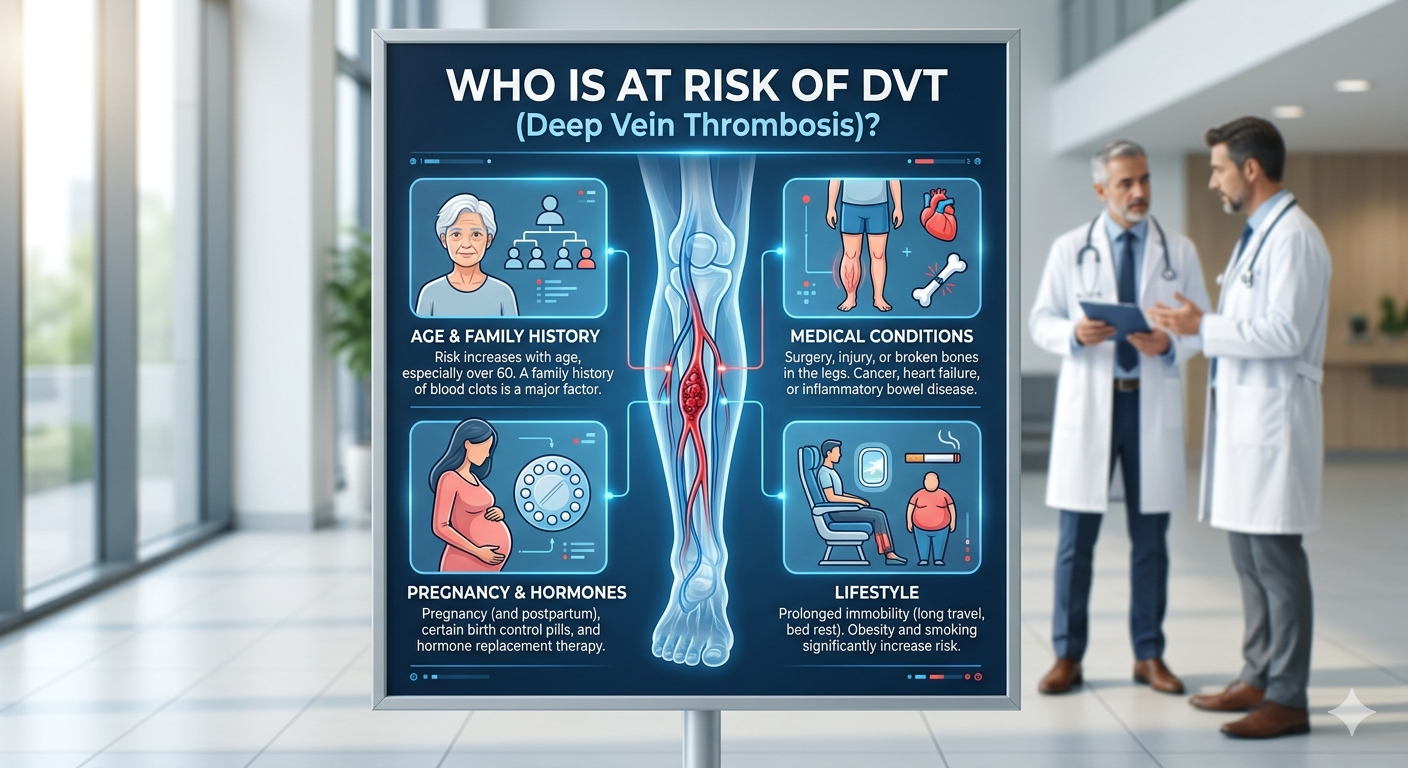
Who Is at Risk of DVT?
- Recent surgery — particularly orthopaedic surgery (hip or knee replacement), abdominal or pelvic surgery. Post-surgical DVT prevention with anticoagulants is standard practice in all major hospitals.
- Prolonged immobility — long-haul flights over 4 hours, extended bed rest, or a limb in plaster cast. Economy class travel over 8 hours increases DVT risk 2–3 fold.
- Cancer — many cancers activate the clotting system. DVT is sometimes the first sign of an undetected malignancy.
- Pregnancy and postpartum period — DVT risk is 5–10 times higher in pregnant women, particularly in the third trimester and the 6 weeks after delivery.
- Oral contraceptive pills or hormone replacement therapy — oestrogen increases clotting factor levels, particularly when combined with smoking.
- Inherited clotting disorders — Factor V Leiden, Protein C or S deficiency, antiphospholipid syndrome. Recurrent DVT without an obvious trigger should prompt testing for these.
- Post-COVID — COVID-19 infection causes a significant pro-thrombotic state. DVT incidence is elevated in patients recovering from COVID-19, particularly those who were hospitalised.
- Obesity and varicose veins — both impair venous return from the legs and increase background DVT risk.
How Is DVT Diagnosed?
Duplex Ultrasound
The primary test. Non-invasive, painless, and highly accurate. Shows the clot location, how far it extends, and whether it is freely floating (mobile clots carry a higher embolism risk). This is the test that confirms or rules out DVT — not clinical examination alone.
D-Dimer Blood Test
A negative D-dimer in a low-probability patient effectively rules out DVT without needing an ultrasound. A positive D-dimer is not diagnostic on its own — it only means something is causing clotting activity (which could be DVT, infection, pregnancy, or many other conditions). Duplex ultrasound confirms.
Wells Score
A clinical scoring system that estimates DVT probability before imaging, based on symptoms, risk factors, and whether an alternative diagnosis is more likely. A high Wells score plus a positive D-dimer means DVT until proven otherwise by ultrasound.
DVT Treatment
Anticoagulation: The cornerstone of treatment. Blood thinners prevent the clot from growing and allow the body to dissolve it gradually. Modern DOACs — rivaroxaban or apixaban — are used in most cases and do not require regular INR blood monitoring, unlike warfarin. Duration is 3 months for provoked DVT (surgery, flight), 6 months or longer for cancer-related DVT or unprovoked recurrent episodes.
Compression stockings: Reduce leg swelling and significantly lower the risk of post-thrombotic syndrome — the long-term venous damage that can follow an unresolved DVT clot.
Catheter-directed thrombolysis: Reserved for large, limb-threatening DVTs causing severe swelling and circulatory compromise — a catheter delivers clot-dissolving drugs directly into the thrombosed vessel.
IVC filter: A filter placed in the inferior vena cava to catch clots before they reach the lungs — used when anticoagulation is contraindicated (recent surgery, active bleeding).
For patients with varicose veins and DVT — both conditions affecting the venous system — Dr. Ved Prakash treats both simultaneously at Yatharth Hospital to address the root cause of recurrent venous disease.
Frequently Asked Questions — DVT Deep Vein Thrombosis Symptoms
What are the classic DVT deep vein thrombosis symptoms?
Unilateral leg swelling, calf pain and tenderness (worse on foot flexion), warmth and redness over the affected calf, and distended surface veins. More than 50% of DVTs are symptomless — which is why high-risk patients require active assessment even without symptoms.
Is DVT dangerous if left untreated?
Yes — untreated DVT carries a 25–30% risk of pulmonary embolism. All proximal DVTs (above the knee) require anticoagulation treatment immediately. Do not wait to see if symptoms improve on their own.
How long after a long flight can DVT develop?
DVT symptoms from flight-related immobility develop within 48 hours to 2 weeks. Risk is highest on flights over 8 hours. Walk every 1–2 hours, wear compression stockings, and stay hydrated on long flights.
How is DVT treated in India?
With direct oral anticoagulants (rivaroxaban or apixaban) in most cases — no regular blood monitoring required. Duration is 3 months for provoked DVT and longer for cancer-related or recurrent unprovoked episodes. Compression stockings are added to prevent long-term venous damage.
Dr. Ved Prakash | Director, CTVS — Yatharth Super Speciality Hospitals, Greater Noida
📞 +91-9355255106 |
📧 drvedprakash@gmail.com |
Book Appointment →


