Varicose Veins — Causes, Symptoms and When They Become Dangerous
Varicose Veins — Causes, Symptoms and When They Become Dangerous
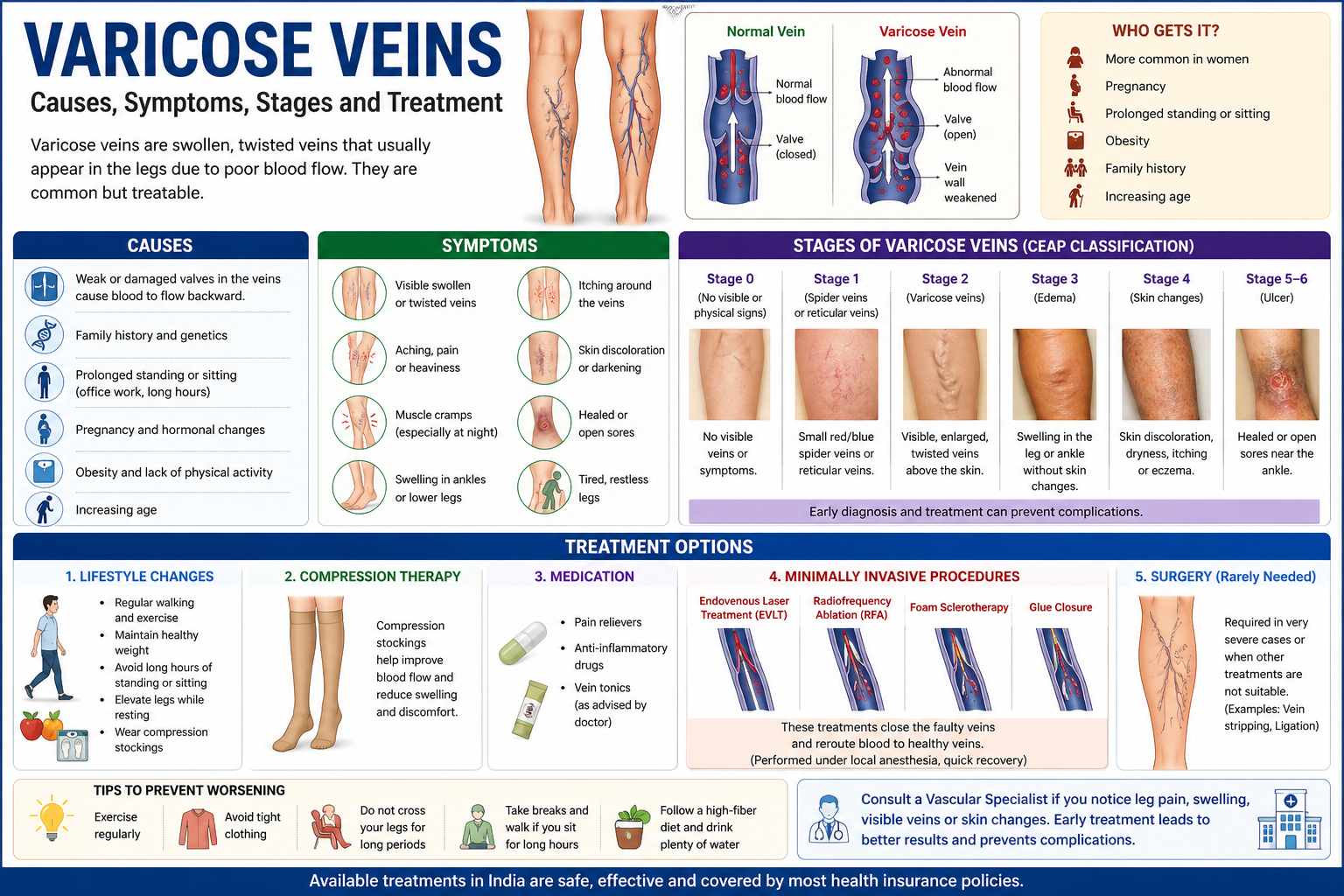
What Are Varicose Veins?
Your leg veins carry blood from the feet back up to the heart — against gravity. To stop blood from flowing backwards between heartbeats, veins contain one-way valves that open as blood flows upward and snap shut as soon as the heartbeat stops pushing. When these valves weaken or are damaged, blood pools in the vein between beats. The pooled blood stretches the vein wall — and over time the vein enlarges, twists, and becomes visibly distorted under the skin.
This is a varicose vein. It is always caused by valve failure — not by the pressure of standing, not by diet, and not by crossing your legs.
Varicose Veins Causes — Why They Develop
Prolonged Standing or Sitting
The most significant occupational risk factor. Teachers, nurses, surgeons, security guards, factory floor workers, and retail staff who stand for 6 or more hours daily put sustained pressure on their leg vein valves. Over years this weakens the valves. Desk workers who sit for long periods face a different but related problem — pelvic vein compression impairs drainage from both legs.
Family History
If one parent has varicose veins, your lifetime risk is approximately 40%. If both parents do, it rises to 90%. Valve weakness is largely inherited — it is not something you caused.
Pregnancy
Multiple mechanisms combine during pregnancy: blood volume increases by 40–50%, the hormone progesterone relaxes vein walls, and the growing uterus compresses the pelvic veins — all increasing the pressure on leg vein valves. Varicose veins from a first pregnancy often improve partially after delivery. They typically worsen with subsequent pregnancies.
Obesity
Increased intra-abdominal pressure from excess body weight continuously impairs blood return from the legs — accelerating valve deterioration.
Age
Valve elasticity decreases naturally with age. Most symptomatic varicose veins present in patients over 40.
Previous DVT
A past episode of deep vein thrombosis can permanently damage vein valves — causing post-thrombotic varicose veins that are more difficult to treat and more likely to cause skin complications.
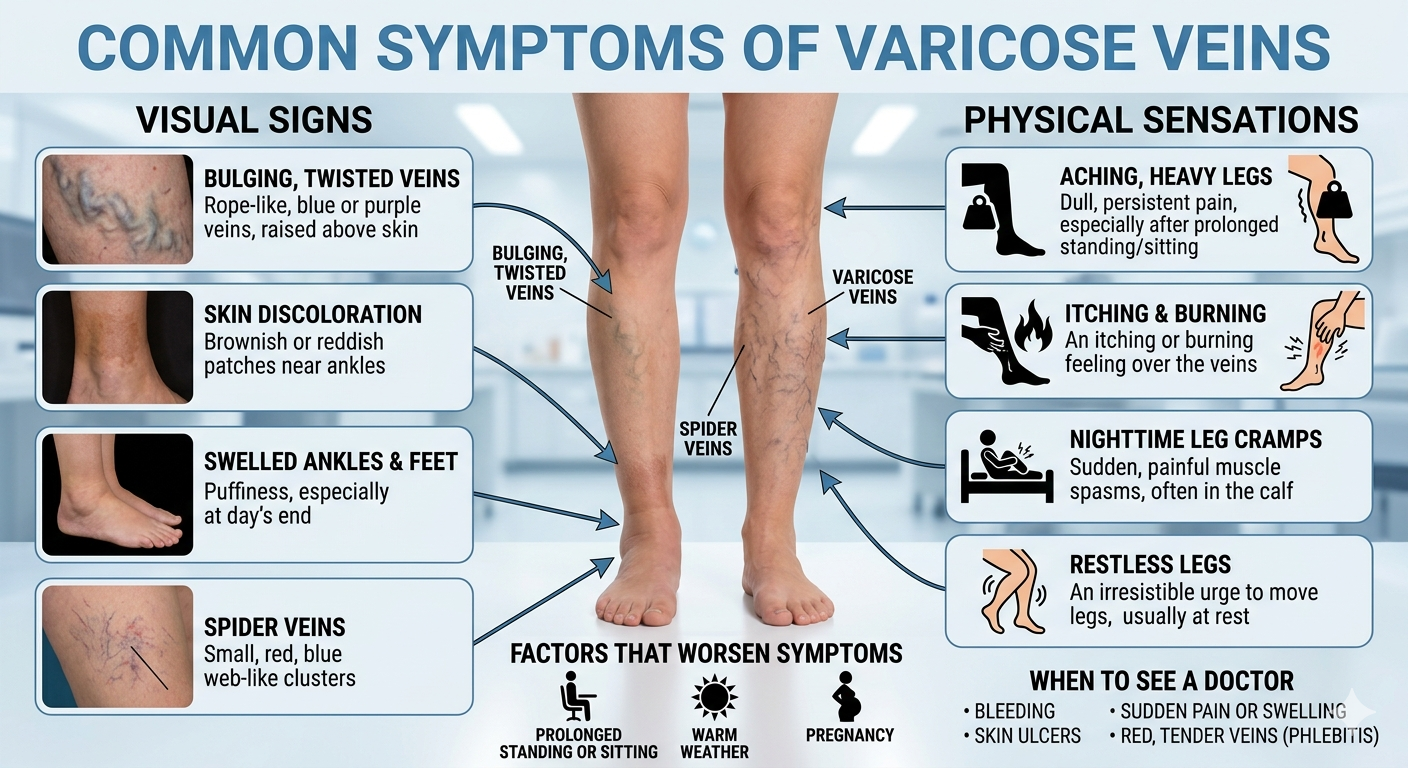
Common Symptoms of Varicose Veins
Varicose veins are usually visible on the legs, but they can also make your legs feel uncomfortable. Common signs include:
Visible Veins
You may notice enlarged veins that look blue or dark purple. These veins often appear twisted, raised, or bulging under the skin, mainly on the legs.
Leg Pain or Heaviness
Your legs may feel tired, sore, or heavy, especially after standing or sitting for a long time.
Swelling
Mild swelling can develop around the feet, ankles, or lower legs, particularly by the end of the day.
Skin Irritation or Changes
The skin around the veins may itch, burn, or feel warm. If not treated, the skin color may slowly become darker.
Leg Cramps
Some people experience muscle cramps or tightening in the legs, often during the night while sleeping.
Varicose Veins Symptoms — Staged by Severity
Varicose veins progress through a clinically recognised staging system called CEAP classification. Understanding where you are in this progression determines urgency of treatment.
C1 — Spider Veins (Telangiectasia)
Small, thread-like red or purple veins visible very close to the skin surface. No symptoms — purely cosmetic. Common in women from their 20s onward.
C2 — Varicose Veins
Bulging, rope-like veins visible under the skin — typically on the calf, back of the knee, or inner thigh. May or may not cause symptoms at this stage. Many patients live with C2 disease for years before seeking help.
C3 — Swelling (Oedema)
Ankle and lower leg swelling that builds through the day and does not fully resolve overnight. This indicates significant venous hypertension — the vein pressure has risen to the point where fluid is being pushed out into the surrounding tissue. At this stage, symptoms include leg heaviness, aching after standing, and cramping at night.
C4 — Skin Changes
Brown pigmentation (haemosiderin staining) around the ankle, eczema over the varicose veins, or a hardening and tightening of the skin above the ankle (lipodermatosclerosis). These are signs of longstanding venous hypertension damaging the skin. This stage requires treatment — it is no longer purely cosmetic.
C5 — Healed Venous Ulcer
A venous ulcer near the inner ankle that has previously healed but left a scar. These patients are at high risk of recurrence without treatment of the underlying varicose veins.
C6 — Active Venous Ulcer
An open wound near the inner ankle that does not heal despite weeks of dressing. This is a medical emergency in vascular terms — it will not close without treating the underlying varicose veins driving the venous hypertension. Referral to a vascular surgeon is urgent.
Primary Causes and Risk Factors of Varicose Veins
Varicose veins develop when the tiny valves inside your veins stop working properly. These valves normally help blood flow upward toward the heart. When they weaken or get damaged, blood flows backward and collects in the veins, making them swollen and visible.
Main Causes and Risk Factors
Age (Getting Older)
As we age, veins naturally lose strength and flexibility. The valves become weaker, increasing the chance of varicose veins.
Pregnancy
During pregnancy, the body produces more blood to support the baby. Hormonal changes and pressure from the growing uterus put extra strain on leg veins, causing them to stretch.
Gender (Women at Higher Risk)
Women develop varicose veins more often than men. Hormonal changes during pregnancy, menopause, or while using birth control pills can affect vein health.
Obesity or Excess Weight
Extra body weight puts additional pressure on leg veins, making it harder for blood to move back to the heart.
Long Periods of Standing or Sitting
Staying in one position for a long time slows blood circulation. Without movement, blood struggles to flow upward against gravity.
Family History
If your parents or close relatives have varicose veins, your chances of developing them are higher.
Previous Vein Damage or Blood Clots
Past injuries, blood clots, or vein problems can damage vein valves and increase the risk.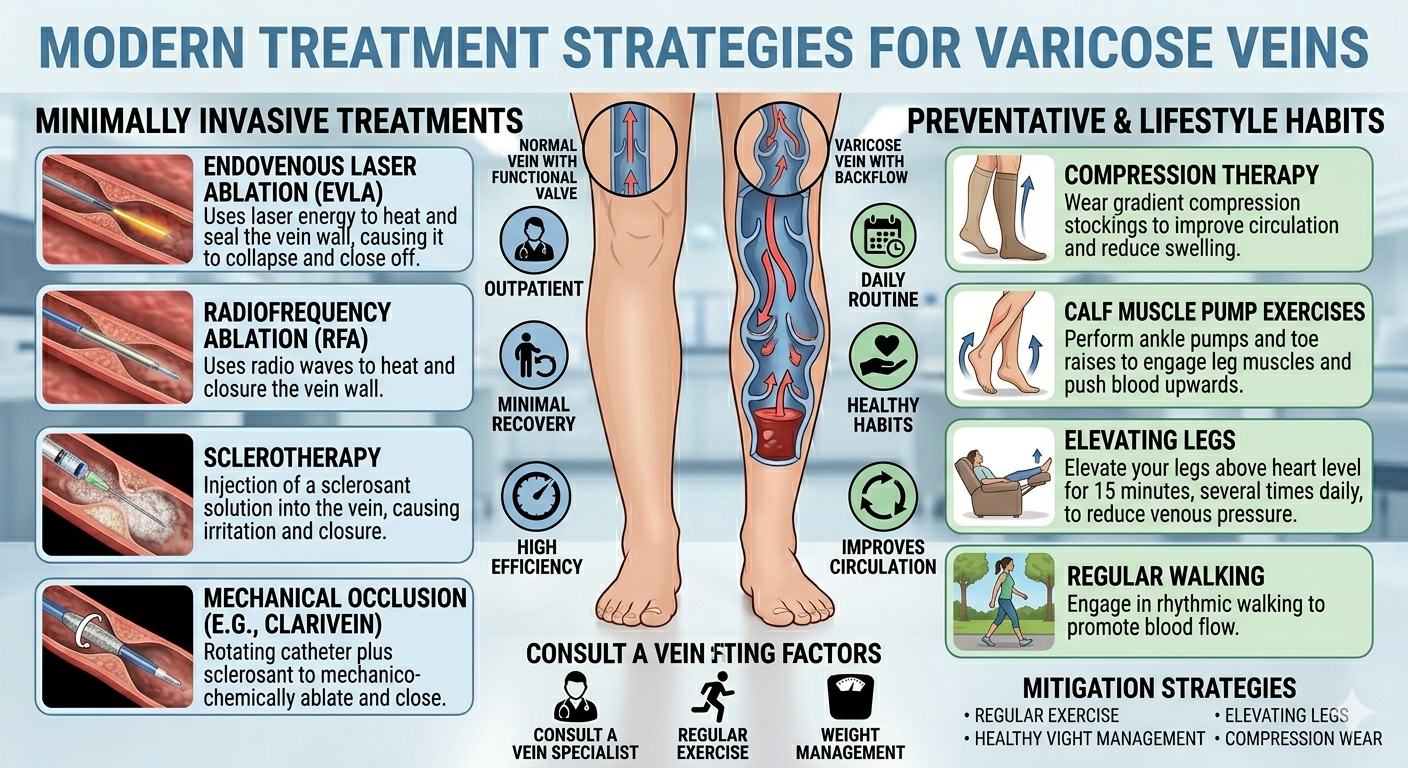
Possible Complications of Varicose Veins
If varicose veins are ignored or not treated for a long time, they may cause some health problems:
Skin Ulcers (Open Sores)
Poor blood circulation can damage the skin around the affected veins. Painful wounds or sores may develop, especially near the ankles, and they can take a long time to heal.
Blood Clots (Inflamed Veins)
Sometimes the veins become swollen and irritated, leading to the formation of blood clots. This condition may cause redness, warmth, pain, or tenderness along the vein.
Bleeding from the Vein
Varicose veins lie close to the skin surface. If a vein gets injured or bursts, it may start bleeding suddenly, even from a small cut or bump.
When Do Varicose Veins Require Treatment?
Treatment is recommended — not optional — when:
- Symptoms significantly affect quality of life at any stage
- Skin changes appear (CEAP C4) — preventing these from progressing to ulceration
- A venous ulcer is present or has occurred previously (CEAP C5–C6)
- A varicose vein has bled — thin-walled varicose veins near the surface can rupture
- Recurrent superficial clots (thrombophlebitis) in the varicose veins
Treatment is available but not medically urgent for purely cosmetic cases at C1–C2 with no symptoms. That said, early treatment at C2 prevents progression to the more serious stages.
For information on the specific procedures used to treat varicose veins — including laser (EVLT) and radiofrequency ablation — visit our page on varicose vein treatment in Delhi NCR.
Frequently Asked Questions — Varicose Veins Causes Symptoms
What are the main causes of varicose veins?
Weakened one-way valves inside the leg veins that allow blood to pool. The main risk factors are prolonged standing (occupational), family history, pregnancy, obesity, and age. Women are twice as likely as men to develop varicose veins.
Can varicose veins go away without treatment?
No — established varicose veins do not resolve on their own. Compression stockings slow progression but do not treat the underlying valve problem. The veins worsen progressively over years without definitive treatment.
Are varicose veins dangerous?
Mild varicose veins are not immediately dangerous but are progressive. Untreated over years they cause skin changes, recurrent bleeding, superficial clots, and venous ulcers. Large varicose veins also increase the risk of deep vein thrombosis.
When do varicose veins need treatment?
Treatment is recommended when symptoms affect daily life, when skin changes appear around the ankle, when a venous ulcer is present or has previously occurred, or when a vein has bled. Cosmetic treatment is available at any stage.
Dr. Ved Prakash | Director, CTVS — Yatharth Super Speciality Hospitals, Greater Noida
📞 +91-9355255106 |
📧 drvedprakash@gmail.com |
Book Appointment →


